- What is deep venous thrombosis (DVT)?
- What are the symptoms?
- What investigations do I need?
- What causes DVT?
- What is the treatment?
- What can I do to prevent this condition?
What is deep venous thrombosis (DVT)?
The veins return the blood from all parts of the body back to the heart. There are three groups of veins in the legs: (i) the superficial veins which are found under the skin, (ii) the deep veins which are found deep in the leg between the muscle groups, and (iii) the perforating veins (or perforators) which connect the superficial with the deep veins. Deep veins lead to the vena cava, the body’s largest vein, which runs directly to the heart.
Deep venous thrombosis (DVT) is thrombosis (clotting) in one or more of the deep veins, usually the ones in the pelvis, thigh or calf and more rarely in the arm, chest or other locations. On the contrary, thrombosis of a superficial vein is called superficial thrombophlebitis and is usually a complication of varicose veins.
It is a potentially serious condition, because it can cause pulmonary thromboembolism. In this condition, a clot breaks free from the deep veins, travels through the bloodstream and blocks the blood flow to the lung(s), and may strain the heart and lung(s). Pulmonary thromboembolism is a medical emergency and may be fatal in a short time.
What are the symptoms?
In half of cases of DVT there are no symptoms. This depends upon the location of the blood clot and its size. The most common symptoms are swelling, tenderness, pain in the leg, which gets worse with standing or walking, sensation of warmth and cyanosis (bluish colour) of the skin.
What investigations do I need?
- A blood test for D-Dimers may be helpful. If negative, it is unlikely that you have DVT.
- Today, the diagnosis is established with duplex ultrasonography of the veins of the leg. This investigation is highly accurate. The best studies are performed by doctors specially trained in vascular ultrasound scanning.
- Venography. Although rarely performed today, it remains the best investigation to confirm or rule out the presence of clots in the veins of the calf.
After the diagnosis of DVT has been confirmed, your doctor may organise more tests to investigate what caused it.
What causes DVT?
It is more likely to develop DVT if you are over 40 years old and obese.
DVT is favoured by three factors: (i) conditions causing blood stagnation in the deep veins, (ii) if the blood is unusually “thick” or “sticky” (as occurs in various hypercoagulable states) and (iii) following an injury to the internal lining of a vein.
Such conditions are:
- prolonged immobilization (during a hospital admission, a long travel by airplane or coach – the “economy class syndrome” etc)
- previous episode of DVT, family history of DVT
- thrombophilia
- malignancy (cancer) or previous malignancy
- operation or trauma, especially of hips, knees, abdomen or chest
- myocardial infarction, stroke, congestive heart failure, inflammatory bowel disease
Also increased risk run women who:
- take oestrogens (contraceptive pills, hormone replacement therapy)
- are pregnant or in puerperium
What is the treatment?
The aim of treatment is to prevent
- death from pulmonary thromboembolism
- recurrence of DVT
- the post-thrombotic syndrome.
In most cases, this is achieved with anticoagulants, like Heparin and Warfarin (or Sintrom). We initially administer some form of Heparin in subcutaneous injections for 5-7 days and then it is decided whether the injection therapy will continue for several months or whether it will be replaced by Warfarin tablets. In recent years, new anticoagulants have emerged. Rivaroxaban (Xarelto), a direct inhibitor of activated factor X (factor Xa), has been licensed for the treatment of DVT and prevention of recurrent DVT in the United Kingdom (www.nice.org.uk/TA261) since 2012, and more recently in Greece. It is given orally and does not require routine anticoagulant monitoring, but is more expensive than Warfarin.
Thrombolytic agents, i.e. drugs injected directly into the clot of the vein with a fine catheter may dissolve even large clots. However, the risk of bleeding (particularly in the brain) is higher than that of anticoagulants, and, therefore, thrombolysis is usually reserved for young people and in special cases, such as quite extensive DVT of the iliac or ilio-femoral venous axis causing significant leg swelling. For safer thrombolysis for DVT in a lower limb, a temporary filter in the inferior vena cava may be inserted prior to the lysis. Permanent inferior vena cava filter insertion has certain indications.
Surgical removal of a vein clot is rarely performed today and only in very serious cases of DVT, when the leg viability is threatened.
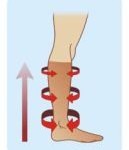
Following an episode of DVT, the use of a graduated compression stocking (of suitable size and class) is highly recommended mainly with the goal to prevent the post-thrombotic syndrome, i.e. chronic venous insufficiency; this may occur as a result of reflux of blood in the veins which have undergone damage in their valves because of the thrombosis.
Generally speaking, the risk of developing post-thrombotic syndrome is reduced if anticoagulation is commenced early after an episode of DVT, and if a compression stocking is properly used for a period of at least two years.
Your vascular surgeon will advise you regarding the type of stocking which is best for you and how it should be used.
What can I do to prevent this condition?
You should avoid standing for long periods of time and having a sedentary life. If you need to remain seated, don’t sit with the legs bent for hours, but stretch your legs out from time to time, and move your feet up and down at the ankles or stand up and stretch your legs. Some data (http://www.nejm.org/doi/full/10.1056/NEJMe1211480?query=OF) indicate that long-term Aspirin intake may reduce the risk of recurrent venous thromboembolism, however, this is not an official guideline-recommendation.
If you are planning to have surgery – Appropriate measures of prophylaxis will be taken by your surgeon depending upon your risk for DVT. These may include anticoagulation, antithromboembolism stockings, early ambulation etc.
If you are planning to travel – Do not wear tight clothes. Move your feet up and down at the ankles, stretch your legs and go for a walk up and down the aisle. Do not get dehydrated: drink plenty of water and avoid alcohol drinks. If you are a person at high risk for DVT, ask your doctor if you need to use compression stockings during your travel or even have Heparin injections.
Επιστροφή
Last modified 07/07/2014