- What are varicose veins?
- What are spider veins (thread veins or venous flares)?
- What causes varicose veins?
- Can pregnancy be the cause of varicose veins?
- What are the symptoms and the complications of varicose veins?
- When should I ask for medical advice and see a vascular specialist?
- Do I need to plan all my pregnancies before I start treatment?
- Do I need to have any investigations for the diagnosis?
- What is the treatment of varicose veins?
- Can varicose veins appear again after the operation?
- Can removal of my varicose veins be harmful?
- What can I do to help myself?
What are varicose veins?
The arteries bring oxygenated blood from the heart to the rest of the body. The veins return oxygen-poor blood back to the heart.
There are three groups of veins in the legs: (i) the superficial veins which are found under the skin, (ii) the deep veins which are found deep in the leg between the muscle groups, and (iii) the perforating veins (or perforators) which connect the superficial with the deep veins.
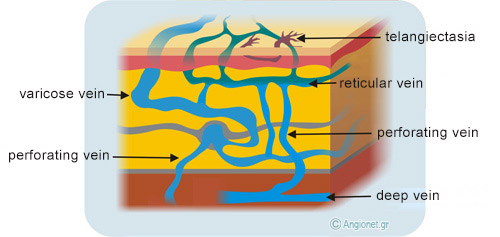
Varicose veins lie in the subcutaneous fat (shown in yellow colour), while telangiectasias (purple colour) lie within the skin and reticular veins (blue-green colour) lie just underneath it.
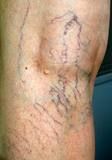
Varicose veins are the result of elongation and swelling of the veins lying under the skin in the suncutaneous fat and usually affect the lower limbs. This swelling of the veins is due to the weakening of the vein wall and the abnormal function of the vein valves (i.e. folds of their lining which should close and prevent blood from flowing backwards towards the feet). Varicose veins occur in the superficial veins and vary in size from the slightly dilated veins to the very tortuous and weak veins; they may cause skin damage in the form of stasis dermatitis and leg ulcers.
For classification of chronic venous disease the system C-E-A-P has been adopted since 1994, where C: clinical signs, E: etiology, A: anatomic distribution, P: pathophysiology. The clinical stages are C0: venous reflux but no visible sign of venous disease, C1: spider veins, C2: varicose veins, C3: varicose veins with oedema, C4, C5, C6: presence of skin changes of increasing severity (without or with venous ulcer). A term used to denote the more advanced form of chronic venous disease (stages C4, C5 and C6) is chronic venous insufficiency.
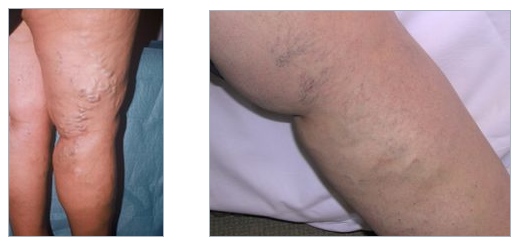
The lower limbs in both photographs are obese with chronic venous disease of CEAP clinical stage C2 (varicose veins). In the leg on the RIGHT, spider veins are more obvious while varicose vein are less prominent.
What are spider veins (thread veins or venous flares)?
Spider veins may be the first sign of increased pressure in the veins of the leg. These are dilated skin veins in the thighs, calves or around the ankles and more rarely in the dorsum of the feet. They usually occur in women of reproductive or older age.
There are two types of spider veins:
- Telangiectasias, which are red-blue or purple intradermal veins (up to 1mm wide)
- Reticular veins, which are green-bluish subdermal veins (1-3mm wide)
Spider veins are mainly a cosmetic problem and rarely cause symptoms, like ache, burning or heaviness in the calf.
The most effective treatment of spider veins is sclerotherapy.
What causes varicose veins?
The normal direction of blood flow in the veins of the legs is towards the heart. There is a series of folds of the lining of the veins, called valves, which open to allow the blood flow towards the heart, and close to prevent blood from flowing backwards to the feet.
If the valves do not function properly, but “leak”, the blood refluxes, i.e. flows backwards to the feet. The pooling of blood increases the pressure in the veins, a condition called venous hypertension. When the superficial leg veins (veins directly under the skin) are affected, this condition is called superficial venous reflux, and may gradually lead to the appearance of varicose veins.
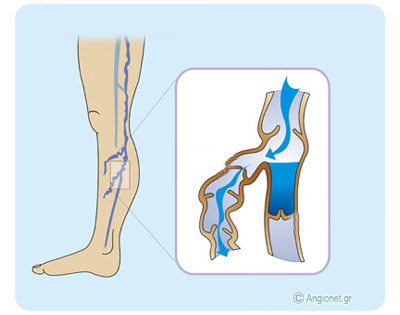
In the inset, the leaking (or incompetent) valves are demonstrated in the vein on the LEFT with the blood refluxing downwards, whereas in the vein on the RIGHT a normal (or competent) valve is shown.
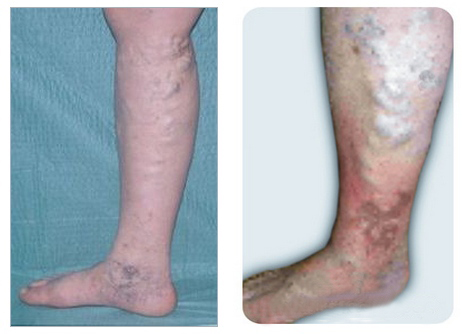
In the photo on the LEFT, chronic venous disease is of clinical stage C2 (varicose veins) according to CEAP classification, while in the photo on the RIGHT it is C4 (varicose veins with skin changes).
The increased frequency of varicose veins causing symptoms in women may have a hormonal cause. It is estimated that 25% of women with varicose veins complain of pain in the legs the days before menstruation. Other aggravating factors are obesity and professions requiring standing for long periods of time.
Apart from the primary, there are the secondary varicose veins, when reflux in the valves of the superficial veins is caused by obstruction of the deep veins of the leg, usually resulting from a previous episode of deep venous thrombosis, and the congenital varicose veins, like Klippel-Trenaunay syndrome ( (a venous malformation).
Can pregnancy be the cause of varicose veins?
It is common for pregnant women to develop varicose veins in their legs, and these seem to cause more symptoms than varicose veins in non-pregnant women. Pregnancy is not the cause of varicose vein formation, but it is a risk factor when there is genetic predisposition to developing varicose veins. Following delivery, varicose veins usually improve within three months. However, if you have consecutive pregnancies, they may remain.
Some pregnant women develop pelvic varices related to venous reflux in an ovarian or an internal iliac (or hypogastric) vein. This type of reflux may cause varicose veins to appear in the vagina, the labia majora of the vulva or the upper part of the medial-back side of the thigh. These varicose veins may be the cause of local discomfort, and usually – but not always – resolve after delivery. If these veins remain, we are in the position today to treat them with a minimally invasive procedure.
What are the symptoms and the complications of varicose veins?
In a high percentage, individuals with varicose veins remain symptom free for a long period of time, even in cases of large varicose veins. On the contrary, other people with smaller veins may have symptoms.
Apart from their unsightly appearance, the commonest symptoms of varicose veins are pain or aching around the veins, burning, itching, numbness and feeling of heaviness in the calf. Occasionally, there may be some oedema (swelling) around the ankles. The symptoms are usually worse at the end of the day and when the weather is warm.
In a few people, the high pressure in the veins causes skin damage in the skin of the gaiter area of the leg, which becomes reddish, brown or black and may develop eczema (or dermatitis). This condition is called chronic venous insufficiency, and if it is allowed to progress, non-healing leg ulcers may appear.
Other complications of varicose veins can be episodes of bleeding through the skin and superficial thrombophlebitis (presenting with redness, pain and induration over an inflamed and clotted vein).
When should I ask for medical advice and see a vascular specialist?
Do not hesitate to see the vascular surgeon even if simply the presence of the swollen veins causes anxiety to you. If you think that you have symptoms related to your varicose veins, it is important that other causes of the symptoms are ruled out, before they are attributed to the varicose veins. If you have any queries, discuss what worries you with your doctor.
More specifically, you need to consult the vascular specialist if you get symptoms like ache, pain, heaviness, burning, itching or swelling; also, if you have developed complications like swelling of a varicose vein which is painful, red or warm to the touch, if a skin eruption has appeared in the lower leg, if there are leg ulcers or if a vein has bled.
Leg varicose veins tend to get worse with time. If you take certain precautions in time, their deterioration may slow down. The earlier you see the vascular surgeon and start treatment, the greater the benefit with regard to your symptoms and the cosmetic result.
Do I need to plan all my pregnancies before I start treatment?
After varicose veins have been successfully treated, they do not come back. This is why it is reasonable that they are treated early. You do not need to finish with all your planned pregnancies before you begin treatment. Of course, new varicose veins may appear in a subsequent pregnancy, but at least the veins already treated will never reappear.
Do I need to have any investigations for the diagnosis?
The diagnosis of varicose veins is easily made by the vascular surgeon by conducting a physical examination and assessing the veins with a continuous wave Doppler. The specialist is qualified to decide whether duplex ultrasonography of the leg veins will be of any additional help and what questions it is called to answer. The best studies are performed by doctors specially trained in vascular ultrasound scanning.
What is the treatment of varicose veins?
For symptom relief and for preventive reasons, you may be recommended to wear graduated compression stockings (or a panty-hose), usually class 1 (18-25 mmHg) or class 2 (25-35mmHg). Compression hosiery is used during the day. It requires replacement by new hosiery every 3-4 months, because of its gradual loss of the degree of compression by use.
For definitive treatment, however, the damaged veins and their connections need to be surgically removed or blocked. The type of varicose vein operation varies from case to case, as the anaesthesia does; the latter can be general, regional or local.
The operation with stripping of the saphenous vein is safe, takes around 60 minutes and the patient is fully mobilised the same day. Some new methods have been developed in recent years, which are less invasive but may also require surgical incisions on the skin of the leg to remove varicosities. They differ in that the saphenous vein is not stripped, but thermally ablated in its place. Thermal ablation methods are radiofrequency closure (RFC) and endovenous laser therapy (EVLT). These methods have some limitations which need to be explained to the patient before the procedure. Another even less invasive method is “chemical ablation” of the saphenous vein, i.e. foam sclerotherapy of the trunk of the saphenous vein under ultrasound guidance, which does not even require local anaesthesia. However, it has limited indications and the results are not uniformley as good as with the aforementioned techniques.
Drug therapy (with venoactive agents) has a rather limited role in the management of varicose veins. It seems, however, that it may offer symptomatic relief in some cases either on its own or together with the use of compression stockings.
With regard to pelvic varices, the method we use today is a minimally invasive technique (venography and embolization of the responsible, or feeding, veins) occasionally in combination with local avulsions or sclerotherapy of the varicose veins.
Can varicose veins appear again after the operation?
Appearance of new varicose veins following a well performed procedure may occur in 20-25% of the cases in a period of 10 years. Occasionally, a new procedure may be required.
Can removal of my varicose veins be harmful?
Varicose veins, as well as spider veins, are damaged veins, which do not function properly. Their removal is not only harmless, but it improves the venous circulation in the leg. From the moment varicose veins appeared, the nearby healthy veins have taken over their work, i.e. returning the blood to the heart.
What can I do to help myself?
Avoid prolonged standing and having a sedentary life. If you need to remain seated for a long period of time, interval walking for a few minutes or flexing the leg will help. Elevate your legs over the heart level, whenever it is possible.
Do not wear tight clothes. Avoid obesity. Avoid exposing your legs to the direct sunlight or other sources of heating.
Follow your doctor’s advice in regard to the use of compression stockings.
EXTERNAL LINKS
- VARICOSE VEINS: AN ANIMATION (VIDEO) http://www.nhs.uk/Conditions/Varicose-veins/Pages/Whatarevaricoseveins.aspx
Last modified 11/11/2014