- What do I need this operation for?
- What does the operation involve?
- Am I eligible for this operation?
- Before the operation
- Coming into hospital
- The operation
- What can I expect after the operation? – Instructions
- Are there any complications?
- What can I do to help myself?
What do I need this operation for?
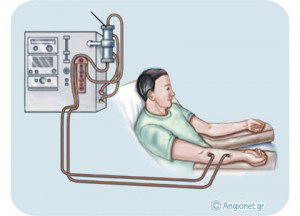
As your nephrologist (or renal physician or kidney disease specialist) has already explained to you, you have a condition called end-stage chronic renal failure, which means that your kidneys have suffered permanent damage so that they cannot clear your blood efficiently from certain toxic substances circulating in it. Your kidney function will be replaced by the dialysis machine (artificial kidney) to which you will be connected 3 times a week.
This connection is performed via two fine and flexible catheters, which will be introduced in your vein through the skin each time. The first catheter (“artery”) will direct your blood to the machine, where it will be filtered. The blood, cleaner now, will be returned to your circulation via the second catheter (“vein”) and through the other puncture site.
The angioaccess (or vascular access) procedures, namely the construction of a fistula or a graft implantation, aim at creating the possibility for the Dialysis Unit staff to have easy access to a vein of yours, which should lie just under the skin and maintain a high blood flow, so that it can be easily and safely punctured.
What does the operation involve?
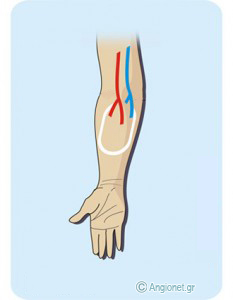
The vascular surgeon will try to identify a suitable superficial vein of an upper limb (forearm or arm) and create high blood flow in it by connecting it with sutures to a nearby artery. This direct arterio-venous communication is called a fistula.
However, if your veins are too thin or scarred by previous punctures for blood taking, IV drug administration etc, the vascular surgeon is very likely to have to implant a graft (plastic tube) under you skin with its one end connected to an artery and the other end to a vein of yours so that a high blood flow is maintained in it.
If your upper limbs are thought to be unsuitable for such a procedure, it can be performed in a thigh or very rarely in other areas of your body.
Am I eligible for this operation?
Apart from a suitable vein, you need to have a suitable artery for sewing without much calcification on its wall. At the same time, the overal arterial circulation to your limb has to be normal without any arterial narrowings, otherwise there is risk for reduction of the blood supply to the limb (arterial steal syndrome) which may cause gangrene of the digits.
The vascular surgeon also will be reluctant to implant a graft if there is an active infection anywhere in your body, because of the risk of graft infection. If graft infection occurs, the graft will have to be removed.
Before the operation
Before selecting the operation site, the vascular surgeon will examine your limbs and may organize a duplex scan for mapping of your arm veins, and rarely a venogram or a digital subtractive arteriogram. You will also be instructed whether you need to discontinue any drug which could increase the risk for bleeding.
Coming into hospital
You will usually be admitted the morning of the day of the operation. You will be asked to have starved for at least 6 hours before the operation, but you may be allowed to have a light breakfast very early in the morning if your operation is scheduled in the afternoon.
When coming into the hospital, it will be very useful to bring along a medical note by your nephrologist stating your medications, any known allergies you may have and any recent blood test results (including your viral antigen profile), chest x-ray or cardiology investigations. You will be asked to sign a form confirming that you understand why the procedure needs to be performed, the risks of the procedure and that you agree to the surgery.
The operation
The operation is usually performed under local anaesthetic, however, the vascular surgeon may ask the anaesthetist to give you light sedation or rarely general anaesthesia.
The vascular surgeon will try to construct the fistula with an incision using the forearm of your non-dominant upper limb. For example, if you are left handed, your physician will place the fistula in your right arm, if possible. To perform the operation, your surgeon joins a suitable vein under the skin to an artery nearby, divides your vein and sews it to an opening made in the side of the artery. As a result, the blood flows down the arteries into the hand, as usual, and also some of this faster moving blood flows into the veins that lead back to your heart. The blood that normally traveled in your divided vein goes back to the heart through other veins, and there is usually plenty of blood remaining in your artery to supply your hand. The vein (now called the fistula) will gradually start to “mature” (i.e. dilate and its wall will become harder), so that in 5-6 weeks it should be suitable for inserting the big needles in it. If it doesn’t mature in a reasonable period, e.g. 3 months, you may need a new operation.
If you cannot receive a fistula because the vein is too thin or blocked, your physician may construct a graft using a tube of man-made, plastic material. Your surgeon sews one end of the graft to one of your veins and the other end to an artery. The graft material will be placed straight or will form a loop under the skin either in your lower arm, upper arm, or less commonly in your leg. Grafts can usually be punctured within 2 weeks.
It is generally preferable to have a fistula than a graft, because it resists to infections and has a better long-term patency, however, if your veins are not suitable, a graft is an excellent alternative.
What can I expect after the operation? – Instructions
- After the operation, you should initially keep the access area raised above your heart to reduce swelling and pain. Your surgeon may recommend an over-the-counter painkiller to relieve pain, if necessary
- Some pain or swelling are frequent and you should not worry as long as they improve. However, if they get worse, you must mention it to your physician immediately, as you should do in case of fever or if the wound leaks or bleeds
- Keep the wound dry for 4-5 days. If you have non-absorbable stitches, these will need to be removed usually in 7-10 days
- Avoid lifting more than about 8 kg or other activities that stress or compress the access area, such as digging
- You should perform exercises to grow and strengthen your fistula, after the pain from the surgery decreases, to make dialysis possible faster and easier. Your physician may recommend squeezing a soft object using the hand on the arm in which the fistula was placed
- You may initially feel some coolness or numbness in the hand with the fistula. These sensations usually go away in a few weeks as your circulation compensates for the fistula. However, if these sensations are severe or do not disappear, tell your physician as soon as possible, because the fistula may be causing too much blood to flow away from your hand, a condition physicians call an “ischaemic steal”
- Grafts mature faster than fistulae, however they have some disadvantages: they are more likely to get infected and tend to last less than fistulae. If you care properly for your graft, however, you can help it last for many years
- Evidently, until the access portal is ready, a catheter in a central vein (usually in your neck) may have to be used for dialysis
Are there any complications?
Potential complications with dialysis access procedures include:
- bleeding
- infection
- stenosis (narrowing) or thrombosis (occlusion) of the access
- limb swelling
- neuropathy
- “ischaemic steal syndrome” discussed above
- aneurysm formation
What can I do to help myself?
Protecting your vascular access is crucial for you!
- Check several times each day that it is functioning. You must be able to feel a vibration called a “thrill”. Your physician or Dialysis Unit staff will be able to show you how to do this
- Monitor for swelling, redness or bleeding after dialysis
- Keep the access site clean
- Do not carry heavy things with the arm which has the access
- Do not sleep on the side of the access
- Do not wear any clothes or jewellery that bind that arm
- Do not let anyone measure your blood pressure on this arm, draw blood or give injections into your fistula or graft
- Do not put any creams or lotions over the site of your fistula or graft – with the exception of Emla cream as a local anaesthetic 1-5 hours before your dialysis
EXTERNAL LINK
- FISTULA FIRST CATHETER LAST: AVF – The first choice for haemodialysis http://fistulafirst.esrdncc.org/ffcl/
Last modified 09/09/2016